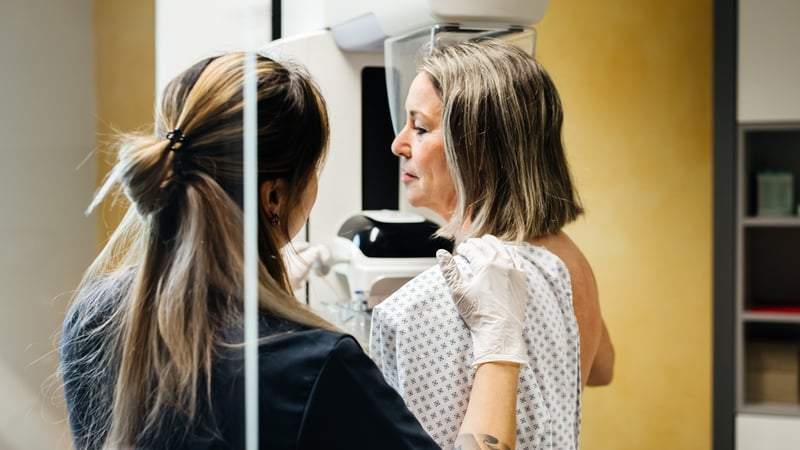
Susan Stone is the creator and presenter of It's a Jungle, exploring the people, science, and ideas shaping our health and wellbeing. Here she investigates the breakthrough science and tech that's reshaping breast cancer detection and treatment.
What if you could check for breast cancer at home in a few minutes? What if a breath test at your GP's office could catch changes between mammograms? What if your doctor knew within weeks - not months - whether your treatment was working?
These aren't hypotheticals. They're technologies in development and early testing right now. And for Irish women - one in seven of whom will develop breast cancer in their lifetime - they could change everything.
But there's a gap between what's possible and what's available. Right now, only about half of eligible women get screened. Many in their 40s have no access at all. And roughly 50% of women have dense breasts, meaning that mammograms can miss a substantial proportion of cancers.
In some studies, up to half of the densest categories - yet most Irish women don't even know if they're in that group.
I spent the past few months speaking to the researchers and entrepreneurs working to close that gap. What I found gave me hope.
Screening You Can Do at Home
Dr Karny Ilan is a general surgeon and the co-founder of Feminai. She sees the problem from both sides - as a clinician treating breast cancer patients, and as an entrepreneur trying to solve the access gap.
"Most women are between stage two and three when they're diagnosed," she tells me. "Earlier detection would mean a very big change, both for the women and for the health system in general. The later you detect breast cancer, usually it means many modalities have to be involved - it's not merely surgery or merely a therapeutic drug. You need a combination of them, which impacts both the patient's quality of life, but also from the economic perspective, it's a very big liability for health systems."
So why aren't more women getting screened? Only about half of eligible women do.
"It usually demands going to medical imaging centres, which for most women are kind of out of the way," Dr Ilan explains. "It means taking at least half a day off just to do it. And specifically women in their 40s and 50s that are super busy - if they're career-focused, if they have families - it's one of those things that would be the first to get pushed down."
Her solution sounds almost too simple: a disposable wearable patch you use at home.
"Through the app, women answer questions - it stratifies them into risk groups and dictates how often they have to do the exam," she explains. "Then the patch itself is disposable, it comes in sizes, and the woman just puts it on. It connects via Bluetooth to the app, she scans herself, it takes a few minutes, and then she tosses it out. The physician receives the results."
Early clinical trials at Sheba Medical Center suggest performance approaching hospital-grade mammography, with around 96% sensitivity and 98% negative predictive value. In simple terms, that means if the patch says there's nothing suspicious, it's very likely to be right.
For women with dense breasts, this could be particularly significant. As Dr Ilan explains: "Very dense breasts - for them, the common screening exams are not as accurate. That's why it's become such a big topic. Women with dense breasts, specifically high-risk women, are looking for other modalities to examine themselves."
Is this meant to replace mammography? Not yet, she says. "Any home devices, at the beginning, have to begin as complementing examinations - there's so much data on big hospital machines. But the whole concept of doing home examinations is shifting the clinical flow and re-educating people on how to take care of themselves. With the hope that in the future it would slowly find its way into the clinical flow."
Feminai recently announced $6 million in seed funding and is currently focused on the US and UK markets, with Dr Ilan hoping for early availability there. For Irish women, it may take longer - but the direction of travel is clear.
"It sends a message that you can control your health," Dr Ilan says. "You don't need to convince anybody that you're feeling something in your breast. You can test yourself."
Her advice for women right now? "Your health comes first. No matter what happens in your life, you have to make sure you're making room and time that prioritises your health. Many times, diseases just come up at you and you weren't prepared. It's all about putting yourself first, no matter what is happening around."

The Breath Test That Could Change Everything
And then there's the approach that sounds like science fiction: detecting breast cancer from your breath.
Karim Aly is CEO of Canadian company Noze, and he's spent years perfecting what he calls "digital odour perception" - essentially teaching machines to smell disease.
"A metabolic odour signature is the chemical fingerprint your body releases in your breath," he tells me. When cells change because of cancer or other diseases, their metabolism shifts, subtly changing the volatile organic compounds (VOCs) that circulate in the blood and are then exhaled.
"Our device isn't 'smelling cancer' per se," he says. "Think of it like a blood test without the needle - instead of drawing blood to read biochemical signals, we smell those signals from your breath."
Dogs proved years ago that disease changes how we smell, but turning that into a tool medicine can rely on is another story. "Dogs proved the biology," Karim says. "The challenge was making it precise, repeatable, and scalable."
Noze's answer is what he calls a "nose-on-a-chip": a miniaturised, ultra-sensitive sensor that detects trace VOCs and builds a molecular map of your breath, then uses AI to interpret the pattern.

"Diseases rarely show up as a single breath molecule," he explains. "They show up as a fingerprint, a pattern across many compounds buried deep in your breath." The technology has space-grade roots, tracing back to NASA's work monitoring astronaut health on the International Space Station.
Dense breast tissue is one of the toughest problems in breast cancer detection, because it can hide
tumours on imaging and make mammograms harder to read with confidence. Breath testing, Karim
argues, has a different edge: "It doesn't depend on anatomy. It reads biology."
Instead of looking for a shadow on a scan, Noze looks for the metabolic fingerprint cancer leaves behind in the breath. In early clinical studies, he says, their test has performed "incredibly well" across the general
population, with accuracy in the same range as mammography - but without the invasiveness, radiation or high cost, and delivering a result in about two minutes. Crucially, performance held up at similar levels in women with and without dense breast tissue, a group in which mammography can be much less reliable.
Right now, their first focus is not to replace mammograms, but to avoid unnecessary biopsies. Among women with suspicious imaging who would otherwise be sent to biopsy, Noze's test showed a 97% negative predictive value.
"That's a very practical number," Karim says. "It means when the breath test says, 'this is unlikely to be cancer', it's right about 97 times out of 100." Longer term, he sees a stepwise path: first reducing unnecessary biopsies, then supporting women with dense breasts alongside mammography, and eventually expanding towards broader screening.

So, when might a European woman see this in her GP's office?
"Developing a new diagnostic approach and getting it approved is a tough journey, and we're tackling it one step at a time," he says. Noze's first clinical breath test is on track "for regulatory clearance in 2026", which would open the door for the wider platform. In breast cancer, they plan to start where the need is most immediate - as an adjunct for women with suspicious imaging, to help rule out unnecessary biopsies
and reduce invasive follow-up - and then move to supporting women with dense breast tissue alongside mammography, before any move towards general screening.
"Europe is absolutely part of that future," Karim says. "So for a European woman reading this: it's coming soon."
For Irish women facing long waits for BreastCheck appointments, or women in their 40s who are
completely excluded from screening, technologies like this could be life-changing. Imagine being able to breathe into a device at your GP's office between mammograms, catching changes early when they're most treatable.

A Wake-Up Call From Someone We Know
Last year, TV presenter Davina McCall announced she'd been diagnosed with breast cancer. For many of us, Davina represents health and vitality - she's been a champion of women's health, particularly around menopause, for years. But what's striking about Davina's story is how she found the lump. She noticed signs in studio toilets - put up by Lorraine Kelly - reminding women to "check your breasts."
Every time she went to the bathroom, she checked. The lump was still there. A biopsy confirmed breast cancer. She had a lumpectomy, caught it very early, and had five days of radiotherapy as a precaution. Davina also mentioned something crucial: she has dense breasts, meaning more fibroglandular tissue and less fat, which can make mammograms harder to read.
She'd had a mammogram but had been postponing the ultrasound. "I just couldn't find time to do it," she admitted. "Don't do that. Get the ultrasound."
Her message is clear: get checked if you're worried. Don't delay your scans. Know your breasts. Her story is exactly why dense breast notification - and better tools for women whose mammograms are harder to read - matter so much.

The Irish Reality
One in seven Irish women will develop breast cancer in their lifetime. It remains the most common cancer diagnosis among women in Ireland. Our national screening programme is under pressure.
Women who should receive their first mammogram at age 50 are now often being called at 52–53, and many women already in the programme are now screened every three years instead of the intended two-year interval.
The age restrictions are equally troubling. BreastCheck covers only women aged 50–69, yet 23% of Irish breast cancer diagnoses occur in women under 50, who have no access to routine screening. The Irish Cancer Society is calling for the screening age to be lowered to 45.
Perhaps most significant is what Ireland doesn't tell women. Unlike the US, which mandated breast density notification in September 2024, Ireland provides no information about breast density after
mammograms.
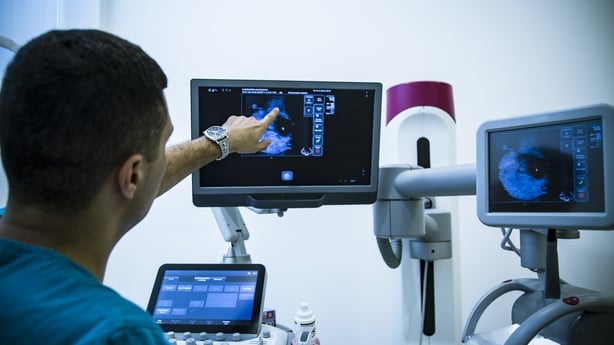
Approximately 50% of Irish women have dense breasts, which both increases cancer risk and can cause up to half of cancers to be missed on standard mammograms. Davina McCall specifically mentioned having dense breasts in her announcement.
Irish women, by contrast, often have no idea whether they fall into this higher-risk category. There is progress happening here. AI is already being piloted at Beaumont Breast Centre, funded by Breast Cancer Ireland, to help radiologists catch subtle cancers - with early results suggesting it may detect up to around 30% more cases than standard reading. But the broader innovations I've described - home screening, breath tests - remain largely unavailable to Irish women for now.
According to the HSE, changes to population-based screening programmes in Ireland, including incorporating breast density into breast screening, must first be evaluated by the National Screening Advisory Committee (NSAC), an independent committee.
The HSE website states that they will "continue to look at the best evidence available to improve screening outcomes for women. As technology improves and more data and research become available, approaches to breast cancer screening may evolve, including for women with dense breasts."
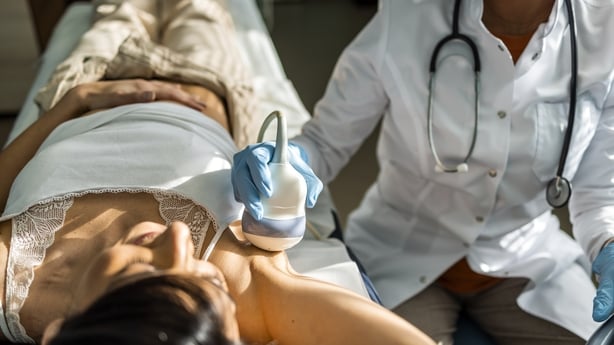
When Diagnosis Is Just the Beginning
What happens after diagnosis? This is where research from an Irish oncologist working in London
offers real hope.
Dr Iseult Browne is a medical oncologist at The Royal Marsden Hospital and The Institute of Cancer Research. Her recent research, published in Clinical Cancer Research, could transform how we monitor breast cancer treatment.
The problem today: when cancer spreads, doctors prescribe treatment and then wait. "Currently, it often takes two to three months, and sometimes longer," Dr Browne tells me. "Patients may spend weeks or months on a treatment before we can be confident it's helping, or before we realise it isn't. That waiting period can be very difficult, both physically and emotionally."

Dr Browne's research shows that a simple blood test could change this. The test measures circulating tumour DNA (ctDNA) - tiny fragments of DNA that cancer cells shed into the bloodstream. "By measuring ctDNA in a blood sample - what we call a liquid biopsy - we can get a real-time snapshot of how active the cancer is," she explains.
"If ctDNA levels fall quickly after treatment starts, it suggests the cancer is responding. If levels stay high or rise, it can be an early warning that the treatment may not be working as hoped."
Her research found that patients whose ctDNA became undetectable after just four weeks were far more likely to respond to treatment and had much longer periods before their cancer progressed. "What stood out was not just the strength of the association, but how consistent it was across different breast cancer subtypes and targeted therapies," she says.
In other words, within about a month of starting treatment, your oncologist could have a reliable signal about whether it's working. If it's not, they can switch to a different approach immediately - rather than waiting months while an ineffective treatment fails.

For Irish women, the timeline is encouraging.
"Ireland is actively involved in major international ctDNA trials and is building national genomic infrastructure," Dr Browne says. "If ongoing trials show that acting on ctDNA results genuinely improves outcomes, this could realistically become part of routine care within the next few years," - although that timeline will depend on trial results and implementation.
Her motivation for this work is deeply personal. "Experiencing cancer at a personal level was a major reason I chose oncology as a specialty," she tells me. "I've seen how the uncertainty of treatment can affect a person's life, their plans, and their sense of control. I wanted to find ways to reduce that waiting, to give patients earlier clarity, and to help them avoid unnecessary side effects when a treatment isn't working."

What To Do Right Now
The technology exists. The validation is there. But it will take time before this becomes standard care in Ireland. So what do you do in the meantime?
Know your breasts. Not just occasionally - regularly. Learn what's normal for you so you can notice changes. Davina's story proves that sometimes the simplest advice is the most powerful. Understand your actual risk.
Ask your GP about a comprehensive risk assessment, not just whether you have a family history. Remember: many women with breast cancer have no identifiable risk factors beyond their age.
Your Action Plan
If you're in your 20s–30s: start tracking how your breasts feel throughout your cycle. Learn what's normal for you. Have baseline conversations with your GP about risk assessment.
If you're in your 40s, don't assume you're "too young" for screening. 23% of Irish breast cancer cases occur in women under 50. If you have concerns or a family history, discuss private screening options or ask for a referral to symptomatic services.
If you're 50+, don't delay BreastCheck appointments. After any mammogram, ask specifically about your breast density. If you have dense breasts, discuss supplemental screening options with your GP.
If you're over 69, you're no longer eligible for BreastCheck, but breast cancer doesn't stop at 69. Continue self-examinations and report any concerns to your GP immediately.
For everyone: check your breasts regularly. Be aware of lumps, swelling, skin changes, or nipple discharge. The earlier you catch something, the better your outcomes.

The Future Is Closer Than You Think
Dr Ilan's wearable patch could enable at-home screening for women who can't access mammography - "I would love to look at us in five years and feel like we've completely changed and revolutionised the way breast health is grasped around the world," she tells me.
Breath tests like Noze's could provide instant results at any point of care. Combined with blood tests like Dr Browne's that ensure you're on the right treatment from week one, we could move from reactive to
truly proactive, personalised care.
And there's more on the horizon. Researchers at MIT are developing AI tools that could potentially identify breast cancer risk from mammograms years before it appears - work I'll be exploring in a future piece. The tools exist.
The question is: will Irish women have access to them?
The future of breast cancer detection and treatment isn't coming. It's here. And while we wait for these innovations to reach Ireland, the most powerful thing you can do costs nothing: know your breasts, trust what you notice, and never let anyone tell you you're too young to be concerned.
This article is for information only and is not a substitute for medical advice. Always discuss screening and treatment decisions with your own doctor.
The views expressed here are those of the author and do not represent or reflect the views of RTÉ.