A new study reports on the effectiveness of a malaria booster vaccine from Oxford University shows long-lasting high efficacy in children in Africa, meeting the World Health Organisation (WHO) specified 75% efficacy goal.
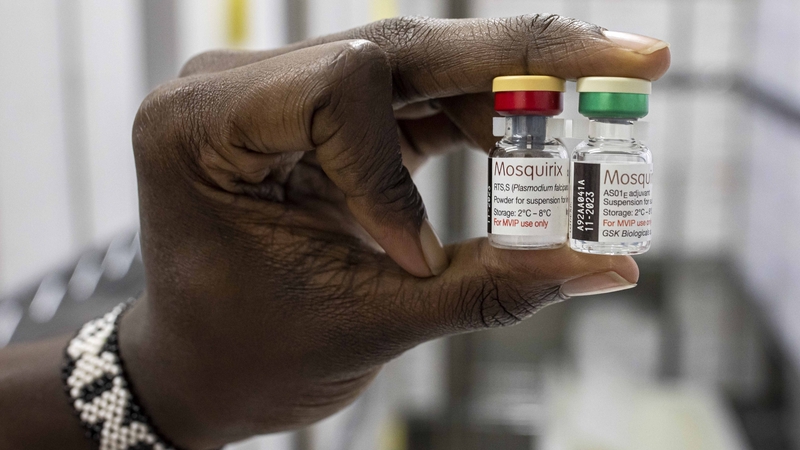
The only approved malaria vaccine Mosquirix, made by global biopharma company GSK, was recently endorsed by the WHO.
GSK has committed to produce up to 15 million doses of Mosquirix every year through 2028, under the roughly 100 million doses a year of the four-dose vaccine the WHO has said is needed long-term to cover around 25 million children.
GSK has said it cannot make enough Mosquirix to meet the vast demand without more funds from international donors.
The Oxford vaccine, called R21/Matrix-M, is likely more effective than Mosquirix in preventing the disease that kills about 600,000 a year despite roughly €3bln spent annually on insecticides, bed nets and anti-malarial drugs, Oxford scientist Adrian Hill said.
It also has a manufacturing advantage, he said, citing a deal with Serum Institute of India to produce 200 million doses annually, starting in 2023.
"We want to add a malaria vaccine on top of nets, on top of spraying, on top of drug preventive treatment.
"If we can do that, and do it at a grand scale, we really could be looking at a very substantial reduction in that horrendous burden of malaria deaths and disease in the coming years - certainly by 2030.
"That's our goal, to make a big impact, maybe a 70% reduction in deaths, we think that could well be feasible."
He added: "We hope that this will be deployed and available and saving lives, certainly by the end of next year."
He said people have been trying to make malaria vaccines for over a century.
"The first clinical trial was in 1940s, 140 different malaria vaccines have been into arms to see if the world can make a vaccine that is useful against malaria.
"We think these data are the best data yet, and very importantly, this is a vaccine that we think can be manufactured and deployed, very widely."
He added that the vaccine could be produced for a few dollars a dose.
Data from a mid-stage study on more than 400 young children who received a fourth dose of the Oxford shot after the primary three-dose regimen showed vaccine effectiveness was 80% in the group that received a higher dose of the immune-boosting adjuvant component of the vaccine, and 70% in the lower-dose adjuvant group, at 12 months following the fourth dose.
The doses were administered ahead of the peak malaria season in Burkina Faso.
Mosquirix versus R21/Matrix-M
The complicated structure and lifecycle of the malaria parasite has long stymied efforts to develop vaccines.
GSK's Mosquirix was conceived back in the 1980s, and paved the way for the Oxford team to create a more potent vaccine, Professor Hill said.
However, it is difficult to make direct comparisons between the two shots, given data from an ongoing larger phase three trial testing the Oxford shot involving 4,800 participants is still to come.
Meanwhile, late-stage trial data published last year showed that if Mosquirix was administered ahead of peak malaria season in high transmission areas, it was nearly 63% effective.
Comparisons between the two vaccines at this stage must be tentative, given they have not yet been compared head-to-head in the same trial, said David Conway from the London School of Hygiene & Tropical Medicine.
However, these phase two data suggest R21/Matrix-M is a step forward from Mosquirix, improving efficacy and the retention of immunity, Alister Craig from the Liverpool School of Tropical Medicine said.
Oxford expects to submit phase three data to the WHO imminently.
With additional reporting from PA.