Analysis: how arthritis plays a stealthy long game with people's lives and what science is doing to out-manoeuvre it
In the 2014 film While We’re Young, the male lead, played by Ben Stiller, receives a shock medical diagnosis in the midst of efforts to relive his youth. As a healthy fortysomething, he expresses disbelief, questioning the doctor as to whether he’s using "arthritis" as a catch all phrase for an injury to his knee. The doctor firmly replies no, that arthritis is degradation of joints. The scene provides a poignant example of how the condition can suddenly interrupt the lives of apparently healthy individuals, leaving them facing a life-long battle.
Symptoms, personal burden and social impact of arthritis
Current figures indicate that over 900,000 people in Ireland live with some type of arthritis making it the biggest cause of disability. If all musculoskeletal conditions affecting the bones and joints are considered together - including back pain, osteoporosis and gout - recent UK estimates suggest up to 29 percent of the population are affected. There are many types of arthritis with a variety of symptoms and severity of effects on bones and joints with the body. Painful, swollen and stiff joints are the main physical symptoms of arthritis and they lead to a substantial reduction in quality of life. Without effective treatment, there is a high risk of permanent joint damage and disability.
We need your consent to load this rte-player contentWe use rte-player to manage extra content that can set cookies on your device and collect data about your activity. Please review their details and accept them to load the content.Manage Preferences
From RTÉ News, a 2013 report on Arthritis Ireland's junior arthritis awareness campaign
At a personal level, a diagnosis of arthritis or a musculoskeletal condition can have a major impact, limiting daily life. Gemma McCooey who has had rheumatoid arthritis for over 30 years describes how it is normal to live with pain. "It may be in my jawbone, toe, hands, arms, elbows, wrists, shoulders, neck, knees or feet. There is always a residual, background pain in my hands and feet. The "good" thing about rheumatoid arthritis is that it is not pain in the same place constantly. The annoying thing is that no matter where the pain is, it is always an obstacle to everyday living."
Everyday tasks can become frustratingly difficult and painful for people with arthritis. "I have no flexibility in my hands or wrists", Gemma explains. "Every day, I use my mouth and teeth to do many of the tasks my hands and fingers used to do. For example, zips and removing the cover inside the cap of the milk container. Modern life does not always make everything easier for everyone."
Those suffering with arthritis can find it more difficult to work. Depending on how relentless the condition is, there can be disruption to normal sleep patterns and lower mood. During "flare ups", when the condition becomes more active, pain can last a week or longer at levels that can make it difficult to leave home, contributing to social isolation. "Arthritis can be very debilitating one day and the next day, after medication and rest, I could be back on my feet", Gemma says. "No-one can see the pain or the difficult times".
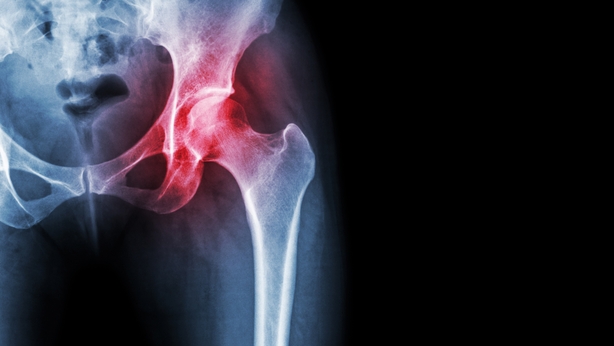
Society is also impacted adversely by arthritis. It has been estimated that the UK loses over 30 million working days per year to musculoskeletal conditions. Healthcare costs for the two most common forms of arthritis (osteo and rheumatoid) are as much as £10.8 billion in UK and €1.6 billion in Ireland per year. "As a result of my condition I was offered early retirement", says Gemma. "I was absent from work for a period of 16 months and was hospitalised a lot during this period. When working, I would go in limping or not able to lift my arms."
Types, causes and treatments
A healthy joint where two bones meet such as the knee provides cushioning support to allow free movement in certain directions. The surfaces of the opposing bone endings are coated with a smooth jelly like substance (cartilage), bathed in a thick lubricant (synovial fluid) and the whole joint enveloped by a fine covering (synovial membrane). The specific triggers and development processes involved in all 200 musculoskeletal conditions are not yet completely clear, but scientific study over the last 50 years has delivered some tantalising clues and new treatments.
Rheumatoid arthritis progresses without symptoms for many years as the natural defence system of the body (the immune system) begins to produce antibodies against self (autoimmunity). Antibodies, normally produced to protect the body against infection, can form complexes within the joint lining. The joint becomes swollen (inflamed) and rapid damage can occur to joints, so an early diagnosis and start to treatment are key.
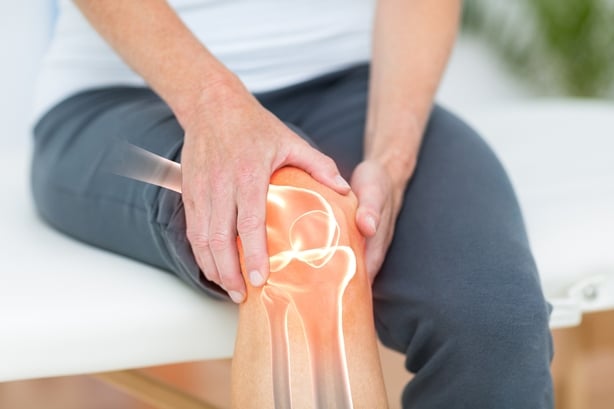
Osteoarthritis is the most common form of arthritis which can affect any joint. Worn cartilage in weight bearing joints, such as the knee, or frequently used joints of the hand, are common place. As cartilage thins, common symptoms joint swelling, pain, knobbly bone growth, stiffness and a reduced range of movement.
Lupus is also an autoimmune condition, where the immune system produces antibodies which attack various parts of the body. The most frequent symptoms are skin rashes, joint pains and extreme tiredness, but people may also experience fever and poor circulation. Around a third of people with lupus can have problems with kidney, heart and lung inflammation.
The onset of these conditions is strongly linked to a range of inherited (genetic) factors which may disrupt regulation of the immune system. Smoking and a high body mass index have also been associated with a higher risk of developing some forms of arthritis. Treatments focus on pain relief, dampening down inflammation and the over active immune system. Specialised biologic drugs which target autoantibody producing cells and inflammatory molecules can be effective in managing the condition.
Key issues targeted by current research
Since a diagnosis of rheumatoid arthritis in her early thirties, Gemma has been prescribed many different pain killers, conventional disease modifying drugs and five biologic medicines. "These medications were very effective for years, with only reactions to a few. They all kept my arthritis at bay and enabled me to enjoy living a great, fulfilled life. I had very few deformities as a result."
Healthcare costs for the two most common forms of arthritis are as much as €1.6 billion in Ireland per year
But recent treatment has not worked so well. "Since then, my hands and feet have become quite deformed and in many ways I am less able to do normal things."
Scientific research efforts worldwide are focussed on addressing a number of challenges which could improve treatment options and quality of life:
(1) Remotely monitoring "flare ups" to allow fine tuning of treatments.
(2) Reducing treatment side effects, such as nausea.
(3) Earlier diagnosis which could to improve chances of effective treatment.
(4) Better ways of selecting high cost treatments which don’t work for all.
(5) More effective pain medication with lower risks of dependence.
(6) How other coexisting conditions such as diabetes may affect treatment (comorbidity).
Future healthcare for people living with arthritis
Armed with a greater understanding of how arthritis arises, we are moving toward a future where prevention or delay of onset may become possible. Genetic testing of individuals with a family history could be used to encourage adjustments in lifestyle. "It is brilliant to know that it may be possible to pre-empt the younger generation developing arthritis through genetic testing", says Gemma.
We are living on the cusp of an era where choosing the right medicine, for the right patient, at the right time is gradually becoming a reality (also known as precision or personalised medicine). Ultimately with scientific progress and participation of individuals in clinical studies, arthritis will have nowhere left to hide.
The views expressed here are those of the author and do not represent or reflect the views of RTÉ