News about studies into the drug Remdesivir has led bulletins across the world over the last 24 hours. Remdesivir is designed to target a specific process which takes place in a cell infected by the virus that causes Covid-19. Understanding that process, and the wider molecular biology of the virus, is what hundreds of scientists are trying to do across the world, to fight the pandemic. Already, they know the virus has weaknesses, and they're trying to find ways to exploit them.
Key to understanding those weaknesses, is understanding the structure of the virus. It may be called 'the invisible enemy' but scientists can set eyes on it, and figure out how it infects our cells. That knowledge of the shape of the virus particle, and the functions of its various bits, underpins nearly all of the drug and vaccine plans that are being developed globally. So understanding the basics, could help you understand a lot of the discussion about Covid-19 in the coming months.
The Virus
Under an electron microscope, the virus looks something like this:
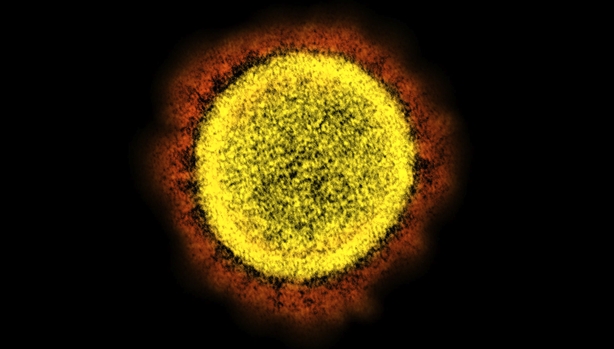
The halo - coloured red here by the US National Institute of Allergies and Infectious Diseases - is a mesh of spikes, which sit on the outside of the virus particle. When it gets into the body, the virus uses those spikes to find a way into certain types of cells which are particularly accessible in our throat and lungs. "Think of it a bit like velcro," says Dr Gerald Barry, a virologist in University College Dublin. "The spikes help it to roll along the cell until it comes across something called the ACE-2 receptor..."
Our Cell
If the ACE-2 receptor on the outside of our cell is the lock, the spike protein on the virus is the key. There's is an interaction between them and an enzyme which acts like a door handle, and that results in the essential bits of the virus particle entering our cells, in other words: infection of the cell.
RTE's graphic designer, Pavels Lavrinovics, drew it up like this:
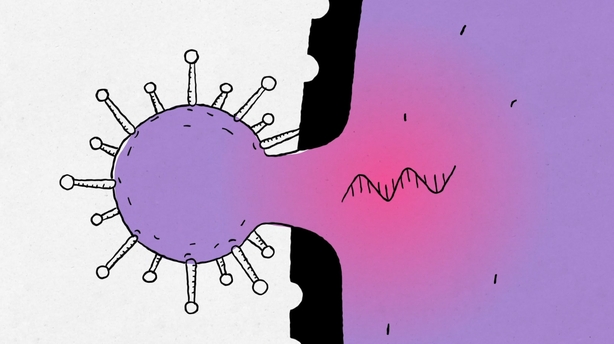
That squiggly line there is the viral RNA, and it's the most important part of the virus. RNA usually manages how the others parts of the cell function, translating plans set out by DNA. When the virus RNA gets into the cell, it re-assigns every thing to one job - make more virus particles. Instead of the cell doing things to keep our bodies working efficiently, it focuses on making viruses. One can get in, thousands of virus particles can come out. They infect other cells, and eventually other people. That process happens over and over again, and you've a global pandemic.
The new viruses are made by the interaction between the RNA and a thing called a polymerase. "The polymerase binds on to the RNA, and effectively acts like a photocopier", says Dr Barry. Stopping that photocopying process is what a lot of the drugs being trialled and tested across the world are trying to do. They're called antivirals because they stop the viral replication.
Antiviral drugs
A lot of hope for a quickly-distributed antiviral is being placed in the aforementioned Remdesivir. It is produced by a company called Gilead, and was originally made to fight ebola. It is one of those drugs attempting to inhibit or disrupt the function of the virus polymerase, effectively creating a paper jam in the photocopier. The polymerase is seen as a particularly exploitable weak spot, because it's part of the virus, not the body. Other drugs being looked at - there's hundreds - are trying to prevent the key (the spike protein) getting into the lock (the ACE-2 receptor), or stop the door handle from working - which relates to the function of an enzyme called TMPRSS2.
But an antiviral may not work effectively in patients whose systems have already been overwhelmed by the virus. They would prevent cases becoming severe, but severe cases need something else. That's down to how the body's immune system reacts to the infection.
The immune response
In 80% of cases, the immune system fights off the infection and in the process develops some form of antibodies to recognise the virus, in case it comes back - we don't know how long those antibodies stay in the system, but we know some get made.
In some of the other 20% of cases, things get complicated when our immune system enters panic-mode. As Dr Kim Roberts, a virologist in Trinity College Dublin puts it, "the immune response is disproportional, and it's the immune response that then starts to cause a lot of the damage."
This combination of virus and immune system overreaction can leave us open to other types of infection, and our lungs unable to properly function, requiring ventilation. So scientists are also working to find a drug to calm the right part of the immune system before it starts to do damage. In Queens University Belfast, Profesor Ultan Power is part of team comparing and assessing available drugs, to see if certain combinations could work. "If we can identify a drug, that doesn't interfere with the other adaptive immune response" he says, "our hope is that we will not impact on the development of good protective immunity, but we will have a very significant impact on the inflammatory response."
Both types of drugs would be for people who are already infected, while vaccines are being made to prevent infections. The WHO is monitoring more than 70 potential vaccines. Again, the structure of the virus is fundamental to how they are being made.
Vaccine design
Some of the candidate vaccines involve hugely weakening the virus, before putting it in to body. The idea being to stimulate the immune system to create enough of the right type of antibodies to be ready to fight the real thing.
Others involve finding a way to get a virus particle that our systems can easily fight off, and get that to carry the spike protein from SARS-CoV2, the virus that causes Covid-19. The idea being our cells which make antibodies will learn to recognise the shape of the spike protein (the key), and be ready to stop it entering the ACE-2 receptor (the lock) when it arrives on the real virus particle. In Oxford University, Irishman Professor Adrian Hill is heading a team using a this method. Many people see them as current leaders in the race to develop a vaccine to stop the virus.
And a final truly modern method is being worked on by several companies, including US-based Moderna. It involves cutting up the RNA of the virus - i.e. clipping up the page before it's put into the photocopier. The aim being to isolate the bit of the virus RNA that makes the spike protein, and get that into our cells. Our cell machinery will then 'photocopy' the spike protein, but never see the rest of the virus particle. Those spikes will be recognised by the immune system, which will make antibodies, ready for a time when the spikes arrive on the virus particle. These are known as RNA vaccines, and many experts believe they will be key to fighting infectious diseases in the years to come, but the technology to produce them has only become viable in the last few years, and none have yet been rolled out. Once approved, they would be very quick to produce, but testing of such designs - and all designs - would be crucial.
In the meantime, the best way to destroy the virus is a simple one: wash your hands.






