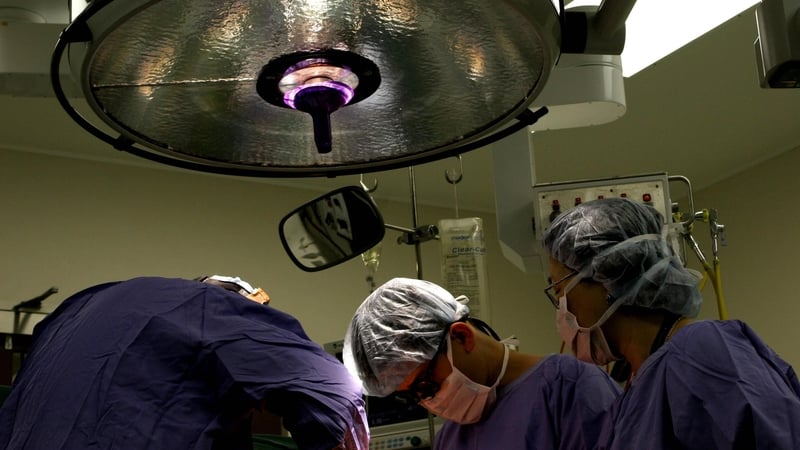
Analysis: the rapid development of new technology is helping with critical decisions in colorectal cancer surgery
By Ronan Cahill, UCD
Think for a minute that you are a patient needing cancer surgery and that you're lying on the operating table just before your anaesthesia. Of course, you want it over as quickly as possible. You want it to be as complete as needed for cure. You also want no more than the cancer alone to be excised so the least impairment results.
Surgeons have long balanced these contradictory requirements. Asking has he or she done the operation before is a good question, but the issue in the surgeon's mind is that it’s the first time you, the patient, are having this surgery. Predictions of the future for any individual is really difficult as we can only apply probabilities from other peoples’ experiences.
Every operation is made up of a series of small components. Both removing a cancer and then reconstructing the remaining tissues comprises many little steps. For everything to go well, each part needs to go well which is why surgeons continually check and confirm correctness of every step serially. This is usually done by subjective measures, best judgement, at a time when there is a lot to consider and the clues are very subtle.
We need your consent to load this rte-player contentWe use rte-player to manage extra content that can set cookies on your device and collect data about your activity. Please review their details and accept them to load the content.Manage Preferences
From RTÉ Radio 1's News At One, Professor Ronan Cahill on the opening of the country's first Digital Surgery Unit at the Mater in 2019
We’ve been working to develop technology to help with such critical decisions in surgery and are already seeing its benefits across the world. It’s also going to get much better soon. In the future, this can involve smart robots and automation. Current robots such as the Da Vinci system right now do nothing to help with visual, cognitive or biophysical interpretations. At present, we are using much simpler, less costly technology to provide decision-support for patients undergoing surgery for colorectal cancer within the time-frame that’s needed in surgery, that is within moments.
Colorectal cancer is important as it’s a common disease that affects about 2,000 people of both genders in Ireland each year. It's second only to breast cancer in women and prostate cancer in men in incidence and to lung cancer in mortality. Surgery is the best chance of cure, but it has some dangers. Any imperfection in intestinal healing after operation risks big consequences including sepsis, septicaemia and peritonitis as the bowel spills its bacteria. Misery as well as organ failure and even death can result and sometimes a bag ('stoma') is needed to reduce or treat these risks. Sadly, these problems happen even in the best of centres.
Most elective colorectal surgery is done now with keyhole or laparoscopic instruments through small (circa 1 cm) incisions. One of these instruments is a camera connected to a computer that allows digital recreation and display of the internal view for all the operating team to see. These images guide their actions and allow decisions to be made. Although it’s been around since the 1980s, we’ve been working hard to really bring this type of surgery into the 21st century by ensuring it is advanced and adapted to help perfect decision-making during surgery everywhere it is done.
Colorectal cancer is important as it affects about 2,000 people in Ireland each year
The first thing we’ve discovered is that using a broader range of light from the camera then just ‘white-light’ helps a lot. By extending the light’s range into the infra-red zone (i.e. just slightly beyond the violet stripe of a rainbow), we can safely see some millimetres into human tissue rather than just reflecting the surface. By also administering via a drip a safe dye that is turned fluorescent by this energy, dynamic blood supply or lymph flow and nodes can be revealed in real-time. This can help ensure conditions in the tissue are as good as possible before attempting to join parts of the bowel back together taking some of the subjectiveness out of it. This is only possible by the computerized camera being primed to detect the energy which is otherwise invisible to the human eye.
Although the basic concepts are quite old, their application in this surgery is new and greatly helped by innovations in optical instrumentation. The dye is really affordable and people rarely have any sort of reaction to it, making it much safer than many other drugs in use. What we’ve seen with this simple technology is that even experts can have their judgment helped as often as in one in every 20 operations. This seems to be particularly the case with patients who would otherwise suffer the most terrible complications. While we are doing an international randomised control trial to definitely prove it, this potentially is the largest increase in safety in this type of surgery that we’ve seen in recent times.
Our better understanding of surgery that has come from this work has further meant that we have begun to apply this concept to identification of cancer tissue during surgery. For the first time, we are able to visually exploit during surgery the fact that cancers possess "angiogenesis" as a hallmark feature (meaning their blood supply is different to healthy tissue) to better personalise the operation.
The patient can have their surgery with all the benefits of the experience continually contributed by surgeons everywhere, to make things better again for each person
This should soon allow surgeons understand better the degree of disease present, even more accurately than that detected by preoperative scans and the unassisted human eye during surgery. By enabling human-machine synergistic collaboration for optimum decision-making, the surgeon can soon be supported by the best of data-analytics available for each case. The patient can have their surgery with all the benefits of the experience continually contributed by surgeons everywhere to make things better again for each person.
To make this a reality, we are working with smart people in every sector. This includes expert surgeons in the Mater Hospital, leading engineers in UCD, talented computer programmers, mathematicians and artificial intelligence specialists in IBM Research, innovative digital pathology developers in Deciphex and major surgical camera manufacturers like Stryker Corporation.
We are working with fantastic applied chemists in the RCSI who can make smarter, more sensitive dyes along. Our network of international surgeons can ensure systems are as good as possible, as safe as possible and that all important details are secure and citizen rights regarding data management are assured. This has all been enabled by the Irish government via Enterprise Ireland through its Disruptive Technologies Innovation Fund. Right now, we've a great tool in use for major cancer operations - and its going to get even better soon.
Prof Ronan Cahill is Consultant Colorectal Surgeon at Mater Misericordiae University Hospital and Professor at the UCD Centre for Precision Surgery at the School of Medicine at UCD.
The views expressed here are those of the author and do not represent or reflect the views of RTÉ